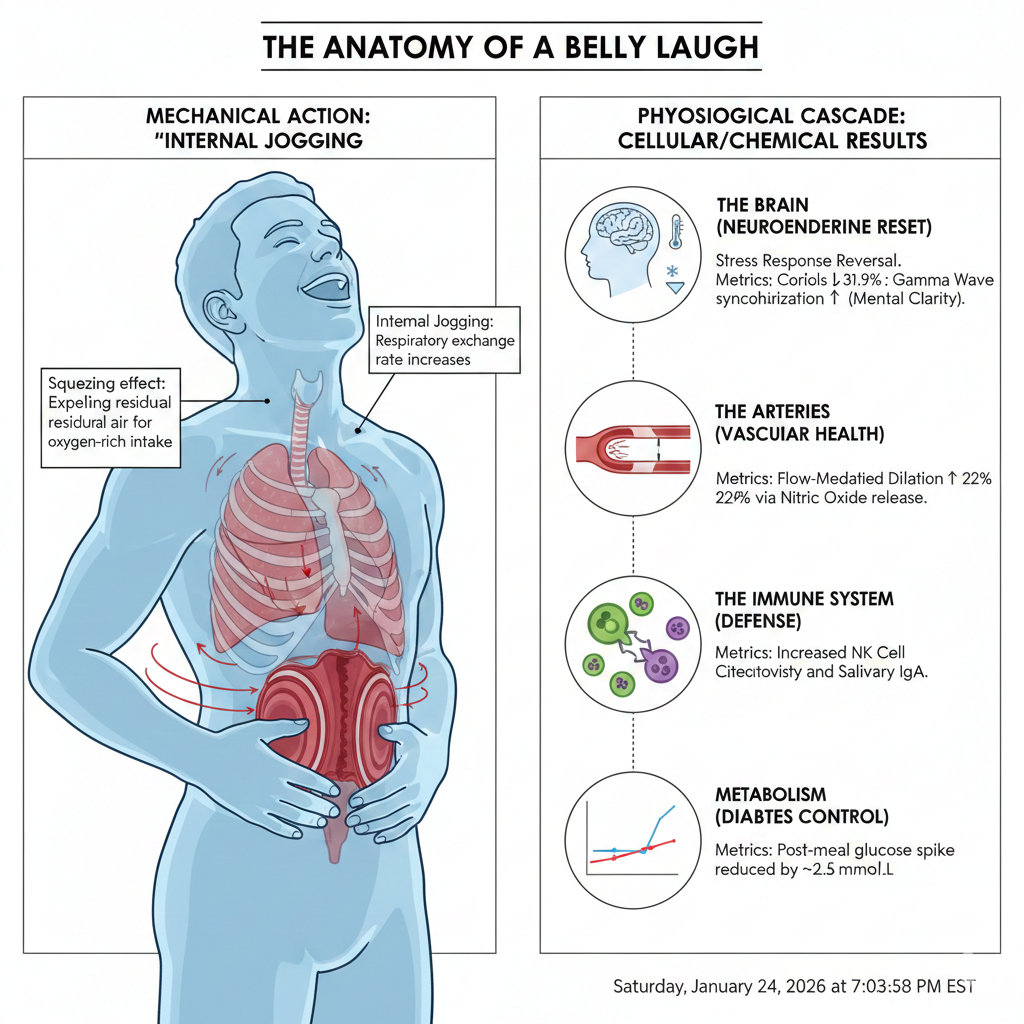
Sexual Health in Men
1. Introduction: Historical Context and Modern Scientific Inquiry
The relationship between male ejaculation frequency and systemic health has been a subject of intense medical, cultural, and philosophical debate for millennia. Historical paradigms often oscillated between the endorsement of regular sexual activity for physiological balance and the admonition of "vital fluid" conservation. In Traditional Chinese Medicine (TCM), the concept of jing (essence) suggests that excessive ejaculation depletes life energy, a theory that parallels the Taoist practices of seminal retention.1 Conversely, 19th-century Western medicine often pathologized masturbation, labeling it a cause of physical debility and mental illness.
However, the last quarter-century (2001–2026) has witnessed a paradigm shift driven by rigorous epidemiological surveillance and advanced molecular biology. The modern scientific consensus has moved away from moralistic or energy-based interpretations toward a data-driven understanding of how ejaculation frequency (EF) acts as a modulator of urological, endocrine, and psychological health. The World Health Organization (WHO) and major urological associations now view sexual function not merely as a reproductive mechanism but as a barometer of overall male health.3
This report provides an exhaustive synthesis of the scientific literature regarding ejaculation frequency. It examines the "dose-response" relationships between ejaculatory emission and prostate carcinogenesis, the physiological trade-offs in semen parameters, the neuroendocrine regulation of stress and immunity, and the psychological correlates of sexual frequency. Furthermore, it stratifies these findings by age, recognizing that the implications of ejaculation frequency in early adulthood differ fundamentally from those in senescence.
1.1 Methodological Scope and Definitions
This analysis integrates data from prospective cohort studies, such as the Harvard Health Professionals Follow-up Study (HPFS) and the European Male Ageing Study (EMAS), alongside randomized controlled trials focusing on reproductive outcomes.
Ejaculation Frequency (EF): For the purposes of this report, EF encompasses all forms of seminal emission, including sexual intercourse, masturbation, and nocturnal emission.
High Frequency: Defined in major epidemiological studies as ≥21 ejaculations per month (EPM).
Moderate Frequency: Defined as 8–12 EPM.
Low Frequency: Defined as 0–3 EPM.
Sexual Health: Defined broadly to include the absence of disease (e.g., prostate cancer), the maintenance of reproductive viability (fertility), and the preservation of psychological well-being.5
2. Epidemiological Analysis: Prostate Cancer Risk and Ejaculation Frequency
The most significant body of research regarding ejaculation frequency pertains to its potential role in the etiology of prostate cancer (PCa). Prostate cancer remains the second most diagnosed cancer in men globally.8 Over the last 25 years, the "Prostate Stagnation Hypothesis" has evolved from a theoretical construct to a biologically plausible mechanism supported by large-scale longitudinal data.
2.1 The Dose-Response Protective Effect
The hypothesis that frequent ejaculation protects against prostate carcinogenesis is rooted in the concept that the prostate gland acts as a bio-accumulator of secretions that, if left stagnant, may become carcinogenic.
2.1.1 The Health Professionals Follow-up Study (HPFS)
The most authoritative data on this subject comes from the Health Professionals Follow-up Study (HPFS), a massive prospective cohort initiated in 1992. Analyzing data from 31,925 men over an 18-year period (and subsequently updated with another decade of follow-up), researchers identified a statistically significant inverse association between ejaculation frequency and prostate cancer risk.5
The findings indicate a clear dose-response relationship:
Risk Reduction: Men in the highest quintile of ejaculation frequency (≥21 times per month) demonstrated a 20% to 33% reduction in the risk of developing prostate cancer compared to the reference group (4–7 times per month).6
Specificity of Protection: The protective effect was most pronounced for low-risk and organ-confined disease. While the association with high-grade, aggressive tumors was less robust in some analyses, the overall reduction in total PCa incidence remains a critical public health finding. The hazard ratios (HR) remained significant even after adjusting for potential confounders such as erectile dysfunction, vasectomy history, and PSA screening frequency.9
2.1.2 Corroborating Evidence and Divergent Studies
A meta-analysis of 22 studies involving 55,490 men reinforced the HPFS findings, reporting that an ejaculation frequency of 2–4 times per week was associated with a significant risk reduction (OR 0.91) compared to lower frequencies.12 Similarly, the CAPLIFE study and Australian cohorts have supported the protective association, particularly highlighting the importance of frequency in early-to-mid adulthood.13
However, the literature is not without nuance. Some earlier case-control studies suggested a potential increased risk associated with high sexual activity in the third decade of life (20s). This discrepancy has been largely attributed to the confounding role of Sexually Transmitted Infections (STIs). High sexual frequency in young adulthood is often a proxy for a higher number of sexual partners. Exposure to pathogens such as Human Papillomavirus (HPV) or Gonorrhea can induce chronic prostatic inflammation, a known risk factor for cancer. When studies control for the number of partners—effectively isolating the act of ejaculation (e.g., via masturbation) from infectious exposure—the protective effect of frequency becomes consistent.15
2.2 Biological Mechanisms of Oncological Protection
Understanding why ejaculation confers protection requires a deep dive into prostatic physiology. The research identifies three primary mechanisms: the clearance of carcinogens, the modulation of crystalloid formation, and the regulation of gene expression.
2.2.1 The Prostatic Stagnation Hypothesis
The prostate gland secretes a fluid rich in citrate, zinc, and enzymes. However, it also concentrates chemical carcinogens from the bloodstream, such as 3-methylcholanthrene, and potentially mutagenic heavy metals. The "Prostate Stagnation Hypothesis" posits that infrequent ejaculation allows these substances to accumulate within the prostatic ductal lumen, increasing the exposure time of the epithelial cells to cytotoxic agents.8
Furthermore, prostatic secretions contain proteinaceous material that can precipitate into corpora amylacea (prostatic concretions) or crystalloids. These intraluminal stones are frequently associated with focal inflammation and proliferative inflammatory atrophy (PIA), a precursor lesion to prostatic intraepithelial neoplasia (PIN) and carcinoma. Frequent ejaculation mechanically flushes the ducts, preventing the formation of these crystalloids and reducing the burden of chronic inflammation.8
2.2.2 Molecular and Genetic Alterations
Moving beyond mechanical flushing, recent research has identified molecular changes associated with ejaculation frequency. A pivotal study utilizing data from the HPFS analyzed tumor tissue and adjacent normal prostate tissue, finding that ejaculation frequency influences the transcriptional landscape of the prostate.
Researchers identified 409 genes that were differentially expressed in the prostate tissue of men with higher ejaculation frequencies. These genes were involved in ubiquitin-mediated proteolysis and cell cycle regulation. The downregulation of pathways associated with cell division and the upregulation of tumor-suppressor mechanisms suggest that frequent ejaculation may create a metabolic environment that is hostile to tumorigenesis.15
2.2.3 Autonomic Nervous System Modulation
A third theoretical framework involves the Autonomic Nervous System (ANS). The prostate is heavily innervated by sympathetic nerves. Chronic sympathetic overstimulation (associated with high tension or unreleased arousal) can accelerate cellular division rates in epithelial tissue. Ejaculation induces a profound shift from sympathetic arousal to parasympathetic dominance (relaxation). This "relief of tension" may slow the turnover of prostate cells, thereby reducing the statistical probability of DNA replication errors that lead to cancer.8
2.3 Age-Stratified Risk Analysis
The relation of age to these results is critical for clinical interpretation. The protective benefit of ejaculation appears to be cumulative, yet specific windows of susceptibility exist.
3. Physiological Dynamics: Semen Quality and Fertility
While the epidemiological data on prostate cancer favors "more is better," the impact of ejaculation frequency on fertility parameters—sperm count, motility, and DNA integrity—presents a complex physiological trade-off. This section analyzes the tension between sperm quantity and sperm quality, challenging historical guidelines on abstinence.
3.1 The Abstinence Interval Debate
For decades, the World Health Organization (WHO) Laboratory Manual for the Examination and Processing of Human Semen recommended an abstinence period of 2 to 7 days prior to semen analysis. This guideline was primarily designed to maximize sperm concentration and semen volume, ensuring that samples from oligozoospermic (low count) men were sufficient for analysis.20
However, the last 15 years of research, driven by the precision requirements of Assisted Reproductive Technology (ART), have revealed that prolonged abstinence is detrimental to sperm function and genetic integrity. The epididymis, where sperm are stored prior to ejaculation, is a biologically active environment. Prolonged storage exposes spermatozoa to reactive oxygen species (ROS) generated by leukocytes and senescent sperm, leading to membrane damage and DNA fragmentation.22
3.2 Sperm DNA Fragmentation (SDF) and Oxidative Stress
Sperm DNA Fragmentation (SDF) is a critical parameter for fertility, strongly correlated with fertilization failure, impaired embryo development, and recurrent pregnancy loss. Modern research overwhelmingly indicates that increasing ejaculation frequency (reducing abstinence) improves SDF.
Mechanism of Improvement: Shorter abstinence intervals (<24 hours) minimize the exposure time of sperm to epididymal ROS. Frequent ejaculation effectively "clears out" older, damaged sperm, ensuring that the ejaculate contains fresh, viable gametes transported recently from the testes.22
Clinical Evidence: A meta-analysis of randomized controlled trials (2010–2025) found that shorter abstinence times were consistently associated with lower SDF levels. In one study, a second ejaculation collected within 1–4 hours of the first showed significantly reduced DNA fragmentation compared to the first sample, making it superior for use in Intracytoplasmic Sperm Injection (ICSI) cycles.25
Reactive Oxygen Species (ROS): Daily ejaculation over a 2-week period was shown to decrease intracellular ROS production in sperm. This reduction in oxidative stress preserves the mitochondrial membrane potential, which is essential for sperm motility and energy metabolism.27
3.3 The Volume vs. Vitality Trade-off
The "cost" of high-frequency ejaculation is a reduction in fluid volume and total sperm count.
Volume Depletion: Daily ejaculation significantly reduces semen volume. The seminal vesicles and prostate require time to replenish seminal plasma. Consequently, total sperm count per ejaculate drops with high frequency. However, studies show that in normozoospermic men, the count plateaus at a level that remains well within the fertile range.27
Motility and Morphology: Crucially, while the number of sperm decreases, the percentage of motile and morphologically normal sperm often increases or remains stable. The "fresh" sperm are more agile and have better acrosome integrity (the cap required to penetrate the egg).30
3.4 Clinical Recommendations for Infertility
The data supports a paradigm shift in managing male infertility. For couples attempting natural conception or undergoing intrauterine insemination (IUI), moderate-to-high frequency (every 1–2 days) is now recommended around the ovulation window to optimize sperm quality, rather than "saving up" sperm, which was the older advice. For men with high SDF, daily ejaculation prior to providing a sample for ART is a validated therapeutic intervention.33
4. Endocrinology: Testosterone, Neurohormones, and "Semen Retention"
The relationship between ejaculation and testosterone (T) is perhaps the most mythologized aspect of male sexual health. Internet communities often promote "semen retention" (abstinence) as a method to skyrocket testosterone levels. Scientific literature, however, paints a picture of homeostatic stability rather than cumulative gain.
4.1 The "Seven-Day Spike" and Baseline Stability
The primary scientific source for the "retention" theory is a 2003 study by Jiang et al., which observed 28 men over a period of abstinence. The study found that on the 7th day of abstinence, serum testosterone levels peaked at approximately 145% of baseline. However, this peak was transient; levels returned to baseline shortly thereafter, regardless of whether ejaculation occurred.35
Subsequent research and longitudinal data have failed to replicate any long-term hormonal advantage to abstinence.
No Cumulative Effect: There is no evidence that abstaining for weeks or months leads to a sustained elevation in baseline testosterone. The body's endocrine feedback loops (Hypothalamic-Pituitary-Gonadal axis) tightly regulate T levels. If levels rise too high, production is downregulated.38
Short-Term Fluctuations: Masturbation and sexual activity can cause acute, short-term fluctuations in testosterone (sometimes a mild increase during arousal), but these are not clinically significant for muscle growth or virility in the long term.39
4.2 Neuroendocrine Regulation: The Benefits of Release
While testosterone remains stable, ejaculation triggers a potent cascade of neurohormones that regulate mood, stress, and bonding.
Oxytocin and Cortisol: Ejaculation, particularly the moment of orgasm, induces a surge in oxytocin. Known as the "bonding hormone," oxytocin has a direct antagonistic effect on cortisol (the stress hormone). This mechanism explains the relaxation and stress relief commonly reported after sexual activity. High-frequency ejaculation, therefore, serves as a repeated biological "reset" for the stress response system.41
Prolactin and the Refractory Period: Ejaculation is unique in stimulating a significant release of prolactin, a hormone associated with satiety and sexual gratification. Prolactin levels are markedly higher after partnered intercourse compared to masturbation (up to 400% higher), which contributes to the "post-coital glow" and the refractory period (time before another erection is possible). This prolactin surge is also a key mediator of the sleep-inducing effects of sex.38
Dopamine: Sexual arousal and ejaculation involve the dopaminergic reward pathways. While "NoFap" proponents argue that frequent ejaculation desensitizes dopamine receptors (downregulation), scientific evidence suggests that in healthy individuals, this system is robust. Pathological desensitization is typically associated with compulsive behaviors (addiction models) rather than frequency itself.38
5. Psychological Dimensions: Mental Health and Sleep
The psychological impact of ejaculation frequency is heavily modulated by the context of the act—whether it is partnered or solitary, and the individual's cultural or moral framework.
5.1 Sleep Quality and Insomnia
Ejaculation is a scientifically validated natural sedative.
Sleep Latency and Quality: A study of over 750 adults found that more than 50% reported improved sleep quality and reduced sleep latency (time to fall asleep) after masturbation to orgasm. This effect is attributed to the "cocktail" of post-orgasmic hormones: prolactin (sedation), oxytocin (relaxation), and vasopressin.
Gender and Context: While both men and women report benefits, men report slightly higher sleep benefits after partnered sex compared to masturbation, likely due to the higher prolactin surge associated with coitus. However, solitary ejaculation remains a highly effective non-pharmacological aid for insomnia.41
5.2 The Guilt-Frequency Paradox
A critical finding in psychological research is that the negative mental health effects often attributed to masturbation (e.g., anxiety, depression) are not caused by the act itself, but by the guilt associated with it.
Ego-Dystonic Masturbation: Men who view masturbation as immoral or "dirty" (often due to religious or cultural conditioning) experience high levels of distress. Studies show that the frequency of masturbation does not correlate with depression, but the guilt regarding masturbation does. High-frequency masturbators who feel no guilt report positive mental health outcomes (stress relief, mood boost), while low-frequency masturbators with high guilt report significant anxiety.46
Compulsive Sexual Behavior Disorder (CSBD): It is vital to distinguish high frequency from compulsion. CSBD is characterized by a failure to control sexual impulses, resulting in repetitive behavior that causes distress or impairment in social/occupational functioning. In these cases, high frequency is a symptom of an underlying impulse control disorder, not the cause of the pathology. The ICD-11 recognizes this distinction, focusing on the distress and lack of control rather than the frequency count.49
6. Immunology and Cardiovascular Health
6.1 Cardiovascular Mortality and Sexual Frequency
The "Caerphilly Cohort Study," a landmark epidemiological project, provided one of the most striking statistics in men's health: men with a high frequency of orgasm (two or more times per week) had a 50% lower risk of mortality from all causes compared to men with low frequency (less than once per month). This association persisted even after adjusting for age, social class, and smoking status.12
Mechanism: This mortality benefit is believed to be a proxy for overall cardiovascular health. Sexual activity acts as mild-to-moderate aerobic exercise (3–5 METs). Furthermore, the capacity to achieve erection and ejaculation is a marker of intact vascular, neurological, and hormonal systems. Men with cardiovascular disease (CVD) who maintain sexual activity often have better prognoses than those who cease activity, although this may be bidirectional (healthier men are more able to have sex).52
6.2 Immunological Modulation
The relationship between sexual frequency and immunity appears to follow a U-shaped or non-linear curve.
Salivary Immunoglobulin A (IgA): IgA is the primary antibody defending mucosal surfaces (mouth, nose) against pathogens. Research on college students demonstrated that those in the moderate-to-frequent group (1–2 times per week) had significantly higher salivary IgA levels (30% higher) than those who were abstinent or those who were extremely frequent (>3 times per week). This suggests that moderate sexual activity stimulates the immune system, while abstinence or potentially excessive exhaustion may not provide the same boost.54
Natural Killer (NK) Cells: Sexual arousal and ejaculation induce a transient leukocytosis (increase in white blood cells), specifically Natural Killer cells (CD3-CD16+CD56+). These cells are crucial for antiviral defense and tumor surveillance. The acute activation of the sympathetic nervous system during arousal releases adrenaline, which mobilizes these immune cells into the bloodstream, potentially enhancing immediate immune surveillance.57
7. Negative Effects and Medical Contraindications
While the benefits of frequent ejaculation are extensive, the literature identifies specific conditions and contexts where it may be detrimental.
7.1 Post-Orgasmic Illness Syndrome (POIS)
POIS is a rare, likely under-diagnosed condition characterized by a cluster of debilitating symptoms appearing immediately or hours after ejaculation.
Symptoms: Severe fatigue, fever, nasal congestion, "brain fog," irritability, and myalgia (muscle pain). Symptoms can last for 2 to 7 days.
Mechanism: The leading hypothesis is an autoimmune or allergic reaction to autologous semen (Type I or IV hypersensitivity) or an imbalance in cytokine release.
Impact: For men with POIS, any frequency of ejaculation is harmful to quality of life. Treatment often involves desensitization therapy (injecting diluted semen) or antihistamines.59
7.2 Epididymal Hypertension ("Blue Balls")
Conversely, the negative effect of not ejaculating after arousal is well-documented. Epididymal hypertension occurs when prolonged sexual arousal leads to vascular engorgement of the genitalia without the release of orgasm. This causes fluid buildup and increased pressure in the epididymis, resulting in testicular pain and heaviness. While not dangerous, it highlights the physiological drive for release inherent in the male reproductive system.62
7.3 The Myth of Nutrient Depletion
A persistent cultural myth is that frequent ejaculation causes nutrient depletion (specifically zinc and protein) leading to hair loss or physical weakness.
Zinc Loss: An average ejaculate contains approximately 2.4 μmol (less than 1 mg) of zinc. The daily recommended intake is 11 mg. While semen is zinc-rich, the amount lost in ejaculation is a fraction of daily intake. Clinical studies show that in men with normal diets, even frequent ejaculation does not cause systemic zinc deficiency. Only in cases of severe malnutrition would this be a factor.65
Protein Loss: The protein content of semen is negligible regarding systemic nutritional status. There is no evidence linking masturbation to muscle wasting or hair loss.68
8. Age-Specific Implications: A Life-Course Perspective
The implications of ejaculation frequency evolve as a man ages, shifting from reproductive concerns to oncological prevention and cognitive maintenance.
8.1 Adolescence and Early Adulthood (Ages 15–29)
Primary Benefit: Establishment of a "low-risk" trajectory for prostate cancer. HPFS data indicates that high frequency (≥21/month) in the 20s correlates with lifetime protection.
Primary Risk: This is the peak age for STI transmission. The "frequency" benefit is negated if it involves unprotected intercourse with multiple partners, as STIs are carcinogenic. Masturbation or safe sex allows for the benefits of frequency without the infectious risk.
Fertility: For young men planning families, high frequency maintains optimal sperm DNA integrity, crucial for healthy conception.10
8.2 Mid-Life (Ages 30–59)
Primary Benefit: This is the critical window for chemoprevention. The prostate is most vulnerable to the initiation of neoplasia during these decades. Regular "flushing" of carcinogens and crystalloids via moderate-to-high frequency (≥21/month) is strongly associated with reduced cancer diagnoses later in life.
Psychological: During these peak stress years (career, family), ejaculation serves as a vital neuroendocrine mechanism for cortisol regulation and sleep hygiene.9
8.3 Late Adulthood and Senescence (Ages 60+)
Primary Benefit: Cognitive and cardiovascular maintenance. Longitudinal studies show that older men who remain sexually active (ejaculating regularly) have slower rates of cognitive decline and better memory function.
Physiological Reality: While the refractory period lengthens and frequency naturally declines, maintaining sexual function ("use it or lose it") is essential for penile tissue health. Regular erections oxygenate the corpora cavernosa, preventing fibrosis and permanent erectile dysfunction.
Mortality: The inverse association with mortality is strongest in this group; sexually active older men live longer, likely due to a combination of physical exertion, hormonal benefits, and the social connectedness often associated with partnered activity.12
9. Conclusion
The synthesis of scientific research from the last 25 years decisively refutes the historical notion of ejaculation as a draining or deleterious act. Instead, the data supports a model where moderate-to-high ejaculation frequency serves as a fundamental mechanism of physiological maintenance for the male body.
Key Findings:
Oncological Protection: Ejaculating ≥21 times per month is associated with a 20–33% reduction in prostate cancer risk across the lifespan. This protective effect is robust, biologically plausible (carcinogen flushing, gene regulation), and cumulative.
Reproductive Superiority: Contrary to older guidelines, frequent ejaculation (abstinence <24 hours) yields sperm with significantly lower DNA fragmentation and oxidative damage, optimizing fertility outcomes despite lower volumes.
Systemic Health: Regular ejaculation correlates with lower all-cause mortality, enhanced immune response (IgA), and improved cardiovascular resilience.
Mental Well-being: Through the release of oxytocin and prolactin, ejaculation acts as a natural anxiolytic and hypnotic (sleep aid), provided it is not accompanied by culturally induced guilt or compulsive pathology.
Negative effects are rare and specific (POIS, STI risk from partners), whereas the myths of testosterone depletion or nutrient loss are scientifically unfounded.
Final Recommendation: For the vast majority of men, maintaining a regular frequency of ejaculation—whether through partnered sex or masturbation—is a positive health behavior. The evidence suggests that "more" (within the realm of ≥21 times per month) is generally "better" for prostate health, genetic fertility, and psychological stress management, establishing frequent ejaculation as a pillar of male longevity and quality of life.
Works cited
Semen and Culture - News-Medical.Net, accessed January 11, 2026, https://www.news-medical.net/health/Semen-and-Culture.aspx
taoist beliefs on ejaculation : r/taoism - Reddit, accessed January 11, 2026, https://www.reddit.com/r/taoism/comments/1munpan/taoist_beliefs_on_ejaculation/
WHO laboratory manual for the examination and processing of human semen, 6th ed, accessed January 11, 2026, https://www.who.int/publications/i/item/9789240030787
Sexuality in Older Adults: Comprehensive Strategies for Clinicians and Patient-Centered Care - PMC - PubMed Central, accessed January 11, 2026, https://pmc.ncbi.nlm.nih.gov/articles/PMC11556589/
Ejaculation Frequency and Risk of Prostate Cancer: Updated Results with an Additional Decade of Follow-up - PubMed, accessed January 11, 2026, https://pubmed.ncbi.nlm.nih.gov/27033442/
Ask the Experts: Does Having More Ejaculations Lessen the Chance of Prostate Cancer?, accessed January 11, 2026, https://www.urologyhealth.org/healthy-living/urologyhealth-extra/magazine-archives/fall-2020/ask-the-experts-does-having-more-ejaculations-lessen-the-chance-of-prostate-cancer
A systematic review of sexual health and subjective well-being in older age groups - NIH, accessed January 11, 2026, https://pmc.ncbi.nlm.nih.gov/articles/PMC9595221/
Does ejaculating often reduce your risk of prostate cancer? - Oncology News Australia, accessed January 11, 2026, https://oncologynews.com.au/latest-news/does-ejaculating-often-reduce-your-risk-of-prostate-cancer/
PD6-07 EJACULATION FREQUENCY AND RISK OF PROSTATE CANCER: UPDATED RESULTS FROM THE HEALTH PROFESSIONALS FOLLOW-UP STUDY - AUA Journals, accessed January 11, 2026, https://www.auajournals.org/doi/10.1016/j.juro.2015.02.802
Ejaculation Frequency and Risk of Prostate Cancer: Updated Results with an Additional Decade of Follow-up - ResearchGate, accessed January 11, 2026, https://www.researchgate.net/publication/299477114_Ejaculation_Frequency_and_Risk_of_Prostate_Cancer_Updated_Results_with_an_Additional_Decade_of_Follow-up
Ejaculation Frequency and Risk of Prostate Cancer: Updated Results with an Additional Decade of Follow-up - PubMed Central, accessed January 11, 2026, https://pmc.ncbi.nlm.nih.gov/articles/PMC5040619/
Sex saves lives | European Journal of Preventive Cardiology - Oxford Academic, accessed January 11, 2026, https://academic.oup.com/eurjpc/article-abstract/29/1/e38/6000660
(PDF) Ejaculation Frequency and Prostate Cancer: CAPLIFE Study - ResearchGate, accessed January 11, 2026, https://www.researchgate.net/publication/370402546_Ejaculation_Frequency_and_Prostate_Cancer_CAPLIFE_Study
New findings on prostate cancer risk and sexual activity - Cancer Council Victoria, accessed January 11, 2026, https://www.cancervic.org.au/about/media-releases/new_findings_on_prostate_cancer_risk_and_sexual_activity.html
Reduction of Prostate Cancer Risk: Role of Frequent Ejaculation-Associated Mechanisms, accessed January 11, 2026, https://www.mdpi.com/2072-6694/17/5/843
Sexual Activity and Risk of Prostate Cancer: A Dose-Response Meta-Analysis - PubMed, accessed January 11, 2026, https://pubmed.ncbi.nlm.nih.gov/30122473/
Sex drive prostate cancer link - ecancer, accessed January 11, 2026, https://ecancer.org/en/news/400-sex-drive-prostate-cancer-link
Ejaculation Changes Prostate Tissue, Lowering Cancer Risk | The Brink | Boston University, accessed January 11, 2026, https://www.bu.edu/articles/2018/ejaculation-changes-prostate-tissue-lowering-cancer-risk/
Does Frequent Ejaculation Reduce Your Risk for Prostate Cancer? - Healthline, accessed January 11, 2026, https://www.healthline.com/health/prostate-cancer/ejaculation-prostate-cancer
Sixth edition of the World Health Organization laboratory manual of semen analysis: Updates and essential take away for busy clinicians - PMC - NIH, accessed January 11, 2026, https://pmc.ncbi.nlm.nih.gov/articles/PMC10929669/
Examination and processing of human semen, accessed January 11, 2026, https://androlog-lab.ru/upload/iblock/491/491a40c6dd9271cfae0128a9cf1968af.pdf
One day is better than four days of ejaculatory abstinence for sperm function - PMC - NIH, accessed January 11, 2026, https://pmc.ncbi.nlm.nih.gov/articles/PMC8812405/
(PDF) Effects of long and short ejaculatory abstinence on sperm parameters: a meta-analysis of randomized-controlled trials - ResearchGate, accessed January 11, 2026, https://www.researchgate.net/publication/381009722_Effects_of_long_and_short_ejaculatory_abstinence_on_sperm_parameters_a_meta-analysis_of_randomized-controlled_trials
Ejaculatory abstinence duration impacts semen parameters - Frontiers, accessed January 11, 2026, https://www.frontiersin.org/journals/endocrinology/articles/10.3389/fendo.2025.1529262/pdf
The Impact of a Very Short Abstinence Period on Assisted Reproductive Technique Outcomes: A Systematic Review and Meta-Analysis - NIH, accessed January 11, 2026, https://pmc.ncbi.nlm.nih.gov/articles/PMC10045034/
Effects of long and short ejaculatory abstinence on sperm parameters: a meta-analysis of randomized-controlled trials - PubMed Central, accessed January 11, 2026, https://pmc.ncbi.nlm.nih.gov/articles/PMC11140051/
Influence of ejaculation frequency on seminal parameters - PMC - PubMed Central, accessed January 11, 2026, https://pmc.ncbi.nlm.nih.gov/articles/PMC4445565/
Can a Short Term of Repeated Ejaculations Affect Seminal Parameters? - PMC - NIH, accessed January 11, 2026, https://pmc.ncbi.nlm.nih.gov/articles/PMC4947206/
Analysis of semen parameters during 2 weeks of daily ejaculation: a first in humans study, accessed January 11, 2026, https://tau.amegroups.org/article/view/11748/html
The Association between Abstinence Period and Semen Parameters in Humans: Results in Normal Samples and Different Sperm Pathology - MDPI, accessed January 11, 2026, https://www.mdpi.com/2075-1729/14/2/188
Effects of long and short ejaculatory abstinence on sperm parameters: a meta-analysis of randomized-controlled trials - Frontiers, accessed January 11, 2026, https://www.frontiersin.org/journals/endocrinology/articles/10.3389/fendo.2024.1373426/full
The Effect of Ejaculatory Abstinence Interval on Sperm Parameters and Clinical Outcome of ART. A Systematic Review of the Literature - MDPI, accessed January 11, 2026, https://www.mdpi.com/2077-0383/10/15/3213
Ejaculatory abstinence duration impacts semen parameters: Insights from a retrospective analysis in male infertility on 23527 analyses - Frontiers, accessed January 11, 2026, https://www.frontiersin.org/journals/endocrinology/articles/10.3389/fendo.2025.1529262/full
Effects of a short abstinence period on sperm quality in oligozoospermic men - PMC - NIH, accessed January 11, 2026, https://pmc.ncbi.nlm.nih.gov/articles/PMC10711244/
A research on the relationship between ejaculation and serum testosterone level in men, accessed January 11, 2026, https://pubmed.ncbi.nlm.nih.gov/12659241/
[Periodic changes in serum testosterone levels after ejaculation in men] - PubMed, accessed January 11, 2026, https://pubmed.ncbi.nlm.nih.gov/12506329/
The Benefits of Not Ejaculating For 7 Days | Good Health by Hims, accessed January 11, 2026, https://www.hims.com/blog/not-ejaculating-for-7-days
Does ejaculation affect testosterone levels? - Examine.com, accessed January 11, 2026, https://examine.com/articles/does-ejaculation-affect-testosterone-levels/
Masturbation and Testosterone: What's the Connection? - Healthline, accessed January 11, 2026, https://www.healthline.com/health/masturbation-and-testosterone
Does masturbation decrease testosterone? - Medical News Today, accessed January 11, 2026, https://www.medicalnewstoday.com/articles/325418
The Health Benefits of Sexual Expression - PMC - NIH, accessed January 11, 2026, https://pmc.ncbi.nlm.nih.gov/articles/PMC10903655/
Perceptions of Sex as a Sleep Promoting Behavior in the General Adult Population - PMC, accessed January 11, 2026, https://pmc.ncbi.nlm.nih.gov/articles/PMC6409294/
First study in decades explores this health benefit of sex - MDLinx, accessed January 11, 2026, https://www.mdlinx.com/article/first-study-in-decades-explores-this-health-benefit-of-sex/lfc-3736
Masturbation Frequency and Sexual Function in Individuals with and without Sexual Partners - MDPI, accessed January 11, 2026, https://www.mdpi.com/2411-5118/3/2/18
How Sex Can Help Improve Your Sleep | Benefits of Sex - Healthgrades Health Library, accessed January 11, 2026, https://resources.healthgrades.com/right-care/sexual-health/how-sex-can-help-improve-your-sleep
Is Ejaculation Frequency in Men Related to General and Mental Health? Looking Back and Looking Forward - PubMed Central, accessed January 11, 2026, https://pmc.ncbi.nlm.nih.gov/articles/PMC8382266/
Masturbation and Anxiety: Is There a Connection? - Healthline, accessed January 11, 2026, https://www.healthline.com/health/masturbation-and-anxiety
Psychological, Relational, and Biological Correlates of Ego-Dystonic Masturbation in a Clinical Setting - PubMed Central, accessed January 11, 2026, https://pmc.ncbi.nlm.nih.gov/articles/PMC5005301/
Evaluation and treatment of compulsive sexual behavior: current limitations and potential strategies - PMC - PubMed Central, accessed January 11, 2026, https://pmc.ncbi.nlm.nih.gov/articles/PMC12268503/
Spotlight on Compulsive Sexual Behavior Disorder: A Systematic Review of Research on Women - Dove Medical Press, accessed January 11, 2026, https://www.dovepress.com/spotlight-on-compulsive-sexual-behavior-disorder-a-systematic-review-o-peer-reviewed-fulltext-article-NDT
Are sex and death related? Study failed to adjust for an important confounder - PMC - NIH, accessed January 11, 2026, https://pmc.ncbi.nlm.nih.gov/articles/PMC1113245/
Cardiovascular Disease and All-Cause Mortality Among Individuals with Low Sexual Frequency - PMC - PubMed Central, accessed January 11, 2026, https://pmc.ncbi.nlm.nih.gov/articles/PMC11898929/
Full article: Sexual activity: an exercise to prevent cardiovascular morbidity and mortality? - Taylor & Francis Online, accessed January 11, 2026, https://www.tandfonline.com/doi/full/10.1586/erc.09.92
Sexual frequency and immunoglobulin A (IgA) | Request PDF - ResearchGate, accessed January 11, 2026, https://www.researchgate.net/publication/8491305_Sexual_frequency_and_immunoglobulin_A_IgA
Sexual frequency and salivary immunoglobulin A (IgA) - PubMed, accessed January 11, 2026, https://pubmed.ncbi.nlm.nih.gov/15217036/
Sexual Frequency and Salivary Immunoglobulin A (IgA) - Semantic Scholar, accessed January 11, 2026, https://www.semanticscholar.org/paper/Sexual-Frequency-and-Salivary-Immunoglobulin-A-Charnetski-Brennan/9d6400082318bbbdb12be1d0d22bab5957aef80a
Effects of sexual arousal on lymphocyte subset circulation and cytokine production in man, accessed January 11, 2026, https://pubmed.ncbi.nlm.nih.gov/15316239/
accessed January 11, 2026, https://www.researchgate.net/publication/8395744_Effects_of_Sexual_Arousal_on_Lymphocyte_Subset_Circulation_and_Cytokine_Production_in_Man#:~:text=The%20results%20confirmed%20transient%20increases,%2B)%2C%20in%20the%20peripheral%20blood.
Post-Orgasmic Illness Syndrome: A Review. - PubMed, accessed January 11, 2026, https://pubmed.ncbi.nlm.nih.gov/29128269/
Postorgasmic Illness Syndrome: What do we know so far?, accessed January 11, 2026, https://www.rarediseasesjournal.com/articles/postorgasmic-illness-syndrome-what-do-we-know-so-far.html
Postorgasmic illness syndrome: potential new treatment options for a rare disorder, accessed January 11, 2026, https://medicaljournalssweden.se/SJU/article/download/11670/15427
Epididymal hypertension: What is blue balls and how do you get rid of it? - Healthy Male, accessed January 11, 2026, https://healthymale.org.au/health-article/what-are-blue-balls-real
Blue Balls (Epididymal Hypertension) Causes and Relief - Verywell Health, accessed January 11, 2026, https://www.verywellhealth.com/understanding-blue-balls-1298225
“Blue balls” and sexual coercion: a survey study of genitopelvic pain after sexual arousal without orgasm and its implications for sexual advances - NIH, accessed January 11, 2026, https://pmc.ncbi.nlm.nih.gov/articles/PMC10155057/
What is the amount of zinc lost per ejaculation during masturbation? - Dr.Oracle, accessed January 11, 2026, https://www.droracle.ai/articles/543232/what-is-the-amount-of-zinc-lost-per-ejaculation
Effects of dietary zinc depletion on seminal volume and zinc loss, serum testosterone concentrations, and sperm morphology in young men - PubMed, accessed January 11, 2026, https://pubmed.ncbi.nlm.nih.gov/1609752/
Association Between Zinc Ion Concentrations in Seminal Plasma and Sperm Quality: A Chinese Cross-Sectional Study - PubMed Central, accessed January 11, 2026, https://pmc.ncbi.nlm.nih.gov/articles/PMC12125066/
How Masturbation Effects Kidney, Stomach, Bones and Back Pain? - Formen Health, accessed January 11, 2026, https://www.formen.health/blogs/sexual-health/how-masturbation-effects-kidney-stomach-bones-and-back-pain
Does Masturbation Cause Protein Loss? & How It Affects Your Hair - Traya, accessed January 11, 2026, https://traya.health/blogs/hair-vitality/does-masturbation-cause-hairfall-and-protein-loss
Impact of ejaculation frequency on semen parameters and DNA fragmentation: a cross-sectional study - PubMed, accessed January 11, 2026, https://pubmed.ncbi.nlm.nih.gov/40671092/
How Often Should A Man Ejaculate: Health Benefits Of Ejaculation - Century Medical Center, accessed January 11, 2026, https://www.centurymedicaldental.com/how-often-should-a-man-ejaculate-health-benefits-of-ejaculation/
Is sex good for your brain? A national longitudinal study on sexuality and cognitive function among older adults in the United States - NIH, accessed January 11, 2026, https://pmc.ncbi.nlm.nih.gov/articles/PMC10615694/
Is Sex Good for Your Brain? A National Longitudinal Study on Sexuality and Cognitive Function among Older Adults in the United States - PubMed, accessed January 11, 2026, https://pubmed.ncbi.nlm.nih.gov/37506374/